Endoscopic Discectomy
 The discs that cushion the spine and allow for normal throughout the day sometimes become damaged due to age-related wear (degenerative disc disease) or injury. Damaged discs may become a source of pain if inner disc material pushes outward through the shell of the disc and presses on nearby nerve roots. If conservative (non-surgical) remedies such as the application of heat or ice, the use of pain-relievers and non-steroidal anti-inflammatory drugs (NSAIDs), and modifying activities aren't effective, surgery may be recommended. An increasingly common procedure is an endoscopic discectomy.
The discs that cushion the spine and allow for normal throughout the day sometimes become damaged due to age-related wear (degenerative disc disease) or injury. Damaged discs may become a source of pain if inner disc material pushes outward through the shell of the disc and presses on nearby nerve roots. If conservative (non-surgical) remedies such as the application of heat or ice, the use of pain-relievers and non-steroidal anti-inflammatory drugs (NSAIDs), and modifying activities aren't effective, surgery may be recommended. An increasingly common procedure is an endoscopic discectomy.
When a Discectomy is Recommended
The first step in determining whether or not an endoscopic discectomy may provide relief is to identify a clear source of back pain or radiating nerve pain (radiculopathy). This process includes ruling out other possible sources of pain with image tests and nerve function tests. The procedure is often recommended when:
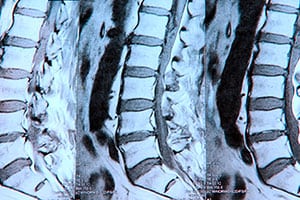
- Disc herniation is the primary source of discomfort
- Other treatment options have been ineffective
- Symptoms from nerve pressure are severe and debilitating
- Related pain is considered chronic (2-3 months or more)
- Radiating nerve pain (especially in legs) lasts 4-6 weeks or longer or is becoming progressively worse
How an Endoscopic Discectomy is Performed
A discectomy is usually performed when the damaged disc is located within the lower (lumbar) spine. The procedure itself involves the removal of all or part of the protruding disc material. The surgery is a minimally invasive operation performed with small incisions and special instruments, one of which is a thin, small camera attached to a tube called an endoscope. During the procedure, the surgeon will be able to view the affected area of the spine on a monitor in the operating room.
A special drill is used to get through the spinal bone to reach the herniated disc and the affected nerve root(s). In some cases, the small piece of bone covering the spine (the lamina) may need to be removed entirely with a procedure called a laminotomy to provide better access to the herniated disc.
After the disc is reached, the damaged part will be removed through the small incision that was created to access the spine. If the entire disc has to removed, an additional fusion procedure may be necessary to stabilize the spine.
Possible Benefits of an Endoscopic Discectomy
 Because smaller incisions are made, patients often experience less bleeding and tissue damage. The use of smaller instruments also means nearby muscles usually don't have to be cut or significantly disturbed while removing the herniated disc material. Patients are often able to actively participate in rehabilitation and physical therapy sooner since there is less healing and trauma involved.
Because smaller incisions are made, patients often experience less bleeding and tissue damage. The use of smaller instruments also means nearby muscles usually don't have to be cut or significantly disturbed while removing the herniated disc material. Patients are often able to actively participate in rehabilitation and physical therapy sooner since there is less healing and trauma involved.
Ideal candidates for minimally invasive procedures like an endoscopic discectomy are otherwise healthy without any significant underlying health issues that may make healing difficult, such as uncontrolled diabetes and high blood pressure. Because of the way the operation is performed, there are typically fewer complication risks. Recovery often includes exercises to restore flexibility and strengthen spine-supporting muscles. Many patients who undergo the procedure are usually able to return to a normal routine within 2-3 months.

